Skin lesions
What are skin lesions?
Skin lesions are abnormal growths or areas of the skin that differ in appearance, texture, or colour from the surrounding healthy skin. They can be flat or raised, small or large, and may have various shapes and colours. Skin lesions can be benign (non-cancerous) or malignant (cancerous), and their causes can range from infections and allergies to sun exposure and genetic factors.
Some common types of skin lesions include:
Moles: Pigmented growths that can be flat or raised, and vary in colour, size, and shape.
Warts: Small, rough-textured, skin-coloured growths caused by human papillomavirus (HPV) infection.
Cysts: Fluid- or semi-solid-filled sacs beneath the skin, often resulting from blocked glands or ducts.
Skin tags: Small, soft, flesh-coloured or brown growths attached to the skin by a thin stalk.
Rashes: Red, itchy, or inflamed areas of the skin, which can be caused by allergies, infections, or irritants.
Pre-cancerous lesions: Abnormal skin cells that have the potential to become cancerous over time, such as actinic keratoses.
Cancerous lesions: Malignant growths that can invade surrounding tissues and spread to other parts of the body. Some cancerous lesions have a tendency to spread to other parts of the body, e.g. malignant melanoma and squamous cell carcinoma. Other may grow locally and destroy normal tissue.
Reasons for Skin Lesion Removal
There are various reasons why someone might consider skin lesion removal, which can generally be categorized into two main groups: cosmetic reasons and medical reasons.
Cosmetic Reasons
Aesthetic concerns are often a primary motivation for skin lesion removal. People may choose to have skin lesions removed for the following cosmetic reasons:
Improving appearance: Skin lesions, such as moles, warts, cysts, or skin tags, can sometimes be considered unsightly or unattractive. Removing these growths can help improve an individual’s self-esteem and confidence in their appearance.
Increasing comfort: Some skin lesions may cause physical discomfort, especially if they are located in areas where clothing, jewellery, or other accessories rub against the skin. Removing these growths can alleviate discomfort and make daily activities more comfortable.

Medical Reasons
In some cases, skin lesion removal may be recommended or necessary for medical reasons, such as:
Preventing skin cancer: Certain skin lesions, such as pre-cancerous growths (e.g., actinic keratoses) or cancerous lesions (e.g., basal cell carcinoma, squamous cell carcinoma, or melanoma), can pose a risk to a person’s health. Early removal and diagnosis can help prevent the spread of skin cancer and improve patient outcomes.
Addressing painful or irritating lesions: Some skin lesions, such as infected cysts or inflamed skin tags, can cause pain or irritation. In these cases, a surgeon may recommend removal to alleviate symptoms and prevent further complications.
Diagnosing uncertain lesions: If a doctor is uncertain about the nature of a skin lesion, they may recommend a biopsy or its entire removal for further examination and analysis. This can help determine whether the growth is benign or malignant, and guide appropriate treatment and follow-up care.
In summary, skin lesion removal may be pursued for cosmetic reasons, to improve appearance or comfort, or for medical reasons, such as preventing or addressing potential health risks. In any case, it is essential to consult with a qualified doctor with experience of treating skin lesions to determine the best course of action based on the individual’s specific circumstances.
Types of Skin Lesions
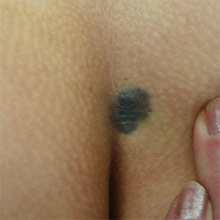
Moles
Moles, also known as naevi, are common pigmented growths on the skin that can vary in colour, shape, and size. They are typically brown or black, but can also be red, pink, or flesh-coloured. Moles can be flat or raised, and may have a smooth or rough texture.
Most moles are harmless and benign, but some may develop into melanoma, a type of skin cancer. Therefore, it is essential to monitor moles for any changes in appearance, such as size, shape, itching or colour, and to consult a healthcare professional if any concerning changes are observed. The ABCDE rule can be a helpful guide for assessing moles:
Asymmetry: If one half of the mole does not match the other half.
Border: If the edges of the mole are irregular or notched.
Colour: If the mole has multiple colours or shades, or if the colour changes over time.
Diameter: If the mole is larger than 6 millimetres or grows in size.
Evolving: If the mole changes in any way, such as shape, size, colour, elevation, or symptoms (itching, bleeding, or crusting).
Moles can appear anywhere on the body, and their number may vary from person to person. Some people may have only a few moles, while others may have many. Moles can develop at any age. Sun exposure, genetics, and hormonal changes can all contribute to the development of moles.
While most moles do not require removal, some individuals may choose to have them removed for cosmetic reasons or if they become irritated or uncomfortable. Various methods can be used for mole removal, including surgical excision, shave excision or cryotherapy.
In cases where a mole is suspected to be cancerous or pre-cancerous, a doctor will recommend its removal for both diagnostic and treatment purposes. The choice of method depends on the size, location, and characteristics of the mole, as well as the patient’s preferences and medical history.
Warts
Warts are small, rough-textured, skin-coloured growths that develop on the skin due to infection with the human papillomavirus (HPV). Warts are non-cancerous and generally harmless, but they can be contagious and may spread to other parts of the body or to other people through direct skin contact or contaminated surfaces.
Warts can appear on any part of the body, but some common types and their locations include:
Common warts: Typically found on the hands, fingers, and elbows, these warts have a rough, cauliflower-like surface.
Plantar warts: Found on the soles of the feet, these warts can be painful and may grow inward due to the pressure exerted while walking or standing.
Flat warts: Smaller and smoother than other types, flat warts often appear on the face, arms, or legs and tend to occur in large numbers.
Filiform warts: Long, narrow growths that commonly appear on the face, around the eyes, mouth, or nose.
Many warts will eventually disappear on their own without treatment, as the immune system fights off the HPV infection. However, this process can take months or even years. Some people may choose to have warts removed due to discomfort, pain, or cosmetic reasons. There are several treatment options available for wart removal, including:
Over-the-counter medications: Topical treatments containing salicylic acid can help break down the wart tissue and stimulate the immune system’s response. These treatments may need to be applied daily for several weeks or months to achieve the desired results.
Cryotherapy: A healthcare provider may use liquid nitrogen to freeze the wart, causing it to blister, die, and eventually fall off. Multiple treatments may be required for complete removal.
Electrosurgery or curettage: The wart is burned off using an electric current or scraped off with a curette, a sharp, spoon-shaped instrument. This method may leave a small scar.
Preventing the spread of warts is important to avoid reinfection and transmission to others. Practising good hygiene, avoiding direct contact with warts, and not sharing personal items such as towels or shoes can help reduce the risk of spreading the virus.
Cysts
Cysts are sacs or pockets filled with fluid, air, or other substances that can form anywhere in the body. They can vary in size and location, from a few millimetres to several centimetres, and may or may not be visible or palpable. Cysts can develop due to a variety of reasons, including infections, genetic conditions, blockages of ducts or glands, or trauma to the skin or tissues.
Some common types of cysts include:
Epidermoid cysts: These cysts develop from skin cells and are filled with keratin, a protein found in hair and nails. They are often small, slow-growing, and painless, and may occur on the face, neck, or trunk.
Sebaceous cysts: These cysts form from blocked oil glands and are typically filled with a yellowish, oily substance called sebum. They can be found on the face, scalp, chest, or back, and may become inflamed or infected if squeezed or irritated.
Ganglion cysts: These cysts develop from joints or tendons and are often found on the wrists or hands. They may appear as small, firm, or rubbery bumps that can be tender or painful.
Pilonidal cysts: These cysts occur at the base of the spine or between the buttocks and are often associated with ingrown hairs or skin irritation. They can become infected and cause pain, swelling, or drainage.
Inclusion cysts: These develop following a puncture wound of the skin.
Most cysts are benign and do not require treatment unless they are causing symptoms or are in a location that interferes with normal function or is cosmetically sensitive. In cases where cysts are painful, infected, or interfere with daily activities, a healthcare provider may recommend cyst removal.
Cyst removal can be performed through various methods, depending on the location and size of the cyst. Surgical excision, aspiration, or drainage may be used to remove the cyst.
Overall, cysts are common and usually benign, but they should be monitored and evaluated by a healthcare provider if they are causing symptoms or concern.
Skin tags
Skin tags are small, soft, benign growths. In areas where they rub against clothing or jewellery they can become irritated. They are composed of loose collagen fibres and blood vessels and may have a stalk or peduncle that attaches them to the skin’s surface. Skin tags can vary in size, shape, and colour, and can occur on any part of the body, but are most commonly found on the neck, armpits, groin, and eyelids.
Skin tags are harmless and do not require treatment unless they are causing discomfort, irritation, or cosmetic concerns. They can be removed through various methods, including:
Snip excision: A doctor will use a sterile scissors or blade to cut off the skin tag at its base after numbing the area with a local anaesthetic. This method may cause minimal bleeding and scarring.
Cryotherapy: A healthcare provider will use liquid nitrogen to freeze the skin tag, causing it to die and fall off. This method can be performed quickly and may not require anaesthesia, but may cause blistering or discoloration.
Electrocautery: A healthcare provider will use a heated wire or needle to burn off the skin tag after numbing the area with a local anaesthetic. This method can be effective, but may cause pain or scarring.
Skin tags are more common in adults. They may also be associated with hormonal changes or genetics. While skin tags are generally harmless, they can be mistaken for other skin growths which may require different treatment. Therefore, it is important to consult with a qualified healthcare provider to determine the nature of the skin growth and the best course of action.
Pre-cancerous and cancerous lesions
Pre-cancerous skin lesions are growths that develop on the skin and have the potential to become cancerous. The most common types of skin cancer are basal cell carcinoma, squamous cell carcinoma, and melanoma. The latter two can be life-threatening if not detected and treated early.
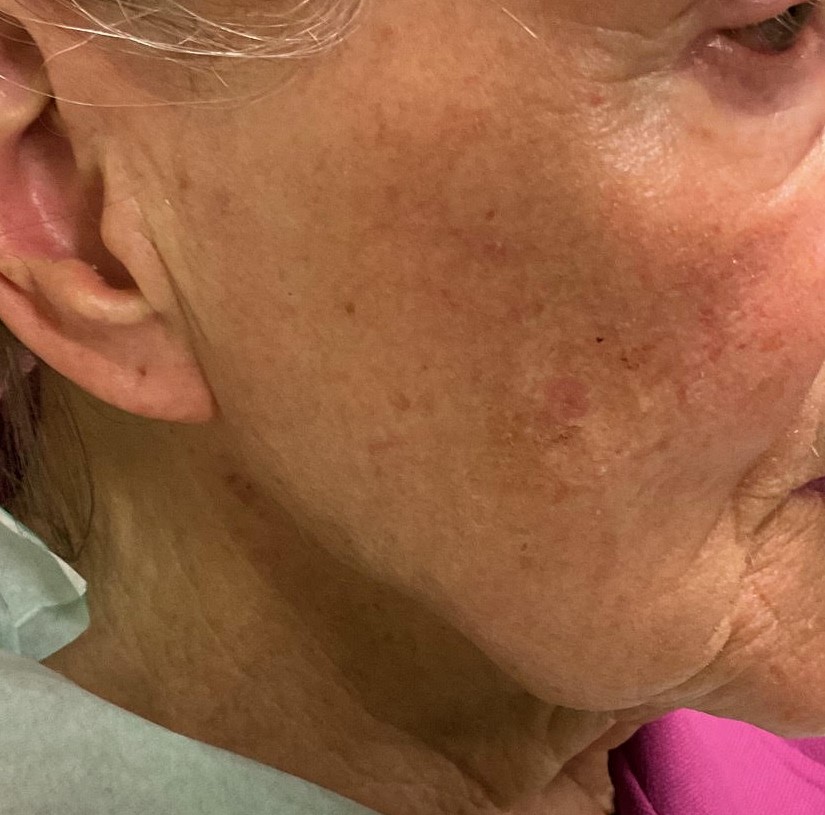
Pre-cancerous skin lesions, also known as actinic keratoses, are scaly or crusty growths that develop on sun-exposed areas of the skin, such as the face, scalp, hands, and arms. They are caused by long-term sun exposure and are considered a warning sign of potential skin cancer. If left untreated, actinic keratoses can progress to squamous cell carcinoma.
Cancerous skin lesions can vary in appearance and may include:
Basal cell carcinoma: This is the most common type of skin cancer and typically appears as a shiny or pearly bump, often with visible blood vessels. It can also look like a scaly, reddish patch or a sore that does not heal.
Squamous cell carcinoma: This type of skin cancer often appears as a firm, red bump or a scaly, crusty patch that may bleed or become ulcerated. It can also develop from pre-existing actinic keratoses.
Melanoma: This is the most serious type of skin cancer and can appear as a dark brown or black mole with irregular borders, multiple colours, and an asymmetrical shape. It can also develop from pre-existing moles.
Skin cancers are often associated with symptoms including itching or bleeding.
Treatment options for pre-cancerous and cancerous skin lesions depend on the size, location, and stage of the lesion. Common treatments include surgical excision, cryotherapy, curettage and electrodesiccation, Mohs surgery, radiation therapy, and chemotherapy. Early detection and treatment are essential for successful outcomes and may involve regular skin checks, self-examinations, and professional skin evaluations.
Prevention of pre-cancerous and cancerous skin lesions includes avoiding excessive sun exposure, using protective clothing and sunscreen, and avoiding tanning beds. Regular skin checks, especially for those with a family history of skin cancer or a personal history of skin lesions, are also important for early detection and prompt treatment.
Diagnosis and Assessment
Diagnosis and assessment of skin lesions involve a comprehensive evaluation of the lesion’s appearance, location, size, and other characteristics, as well as the patient’s medical history, skin type and symptoms. The goal is to determine the nature of the lesion and determine the appropriate course of action, whether it be monitoring, treatment, or referral to a specialist.
The diagnosis and assessment of skin lesions typically involve the following steps:
Medical history: A healthcare provider will ask the patient about their medical history, including any previous skin lesions, family history of skin cancer or other skin conditions, and any symptoms or changes in the lesion.
Physical examination: A healthcare provider will examine the lesion, looking for characteristics such as size, shape, colour, texture, and whether the lesion is raised or flat.
Dermoscopy: A dermatoscope, a handheld device that magnifies the skin’s surface, may be used to examine the lesion in more detail and identify any suspicious features.
Biopsy: A tissue sample of the lesion may be taken for analysis to determine if it is cancerous or pre-cancerous.
Imaging tests: Imaging tests, such as MRI, may be used to evaluate the lesion’s depth and involvement in underlying tissues or organs.
The assessment of skin lesions may involve a classification system, such as the ABCDE method, which stands for asymmetry, border irregularity, colour variation, diameter greater than 6mm, and evolving over time. This method can help healthcare providers determine if a lesion is suspicious and requires further evaluation or treatment.
It is important to seek medical attention if you notice any changes in a skin lesion or if you have a new lesion that concerns you. Early detection and treatment are essential for successful outcomes and may involve regular skin checks, self-examinations, and professional skin evaluations.
Skin Lesion Removal Methods
A skin lesion should be removed if it is causing discomfort, pain, or functional impairment, or if it is suspected to be cancerous or pre-cancerous. The type and extent of surgery depends on various factors, including its size, location, type, and appearance, as well as the patient’s medical history and personal preferences.
Some common reasons for skin lesion removal include:
Cosmetic concerns: Skin lesions, such as moles or skin tags, may be removed for cosmetic reasons if they are located in visible or prominent areas of the body and cause self-consciousness or embarrassment.
Irritation or discomfort: Skin lesions that are constantly irritated by clothing, jewellery, or movement may be removed to relieve discomfort or pain.
Suspicion of cancer: Skin lesions that are irregular, growing, bleeding, or changing in appearance may be removed to obtain a biopsy and determine if they are cancerous or pre-cancerous.
Functional impairment: Skin lesions that interfere with normal body function, such as cysts or lipomas that affect mobility or range of motion, may be removed to improve quality of life.
The method of skin lesion removal depends on the type and location of the lesion, as well as the patient’s medical history and preference.
It is important to consult with a doctor with expertise in ski lesion diagnosis to determine the best course of action for skin lesion removal. Some lesions may not require removal, while others may require prompt attention to prevent complications or serious health problems. Regular skin checks and self-examinations are also important for detecting any changes in existing skin lesions and identifying any new ones.
Surgical excision
Surgical excision is a common method used to remove skin lesions that are suspected to be cancerous, pre-cancerous, or causing discomfort or cosmetic concerns. The procedure involves removing the lesion along with a margin of healthy skin, which is sent for analysis to determine if all cancer cells have been removed.
The surgical excision procedure typically involves the following steps:
Anaesthesia: The patient is given local anaesthesia to numb the area around the lesion. In some cases, sedation or general anaesthesia may be used.
Incision: The surgeon makes an incision around the lesion, ensuring that a margin of healthy skin is included.
Removal: The lesion is removed, along with the surrounding tissue. The wound may be closed with stitches or adhesive strips.
Dressing: A dressing is applied to the wound to protect it from infection and promote healing.
Follow-up: The patient is instructed on wound care, pain management, and signs of complications. A follow-up appointment is typically scheduled to monitor the wound’s healing and remove any sutures.
Surgical excision is a safe and effective method for removing skin lesions, but it may be associated with some risks and complications, including bleeding, infection, scarring, or nerve damage. The risks and benefits of surgical excision are fully discussed before the procedure in my practice..
After surgical excision, the removed tissue is sent for analysis to determine if it is cancerous or pre-cancerous. If cancer is detected, further treatment, such as a wider excision, radiation therapy or chemotherapy, may be recommended to prevent recurrence or spread.
It is important to monitor the wound for signs of infection or complications, such as excessive bleeding, swelling, redness, or discharge. It is also important to protect the wound from sun exposure and avoid strenuous activity until it has fully healed.
Cryotherapy
Cryotherapy is a method of skin lesion removal that involves freezing the lesion with liquid nitrogen or other freezing agents. The procedure is commonly used to remove warts, actinic keratoses, and other benign skin lesions.
The cryotherapy procedure typically involves the following steps:
Preparation: The area around the lesion is cleaned.
Freezing: A small amount of liquid nitrogen is applied to the lesion with a cotton swab or spray gun, freezing the lesion and the surrounding tissue. The freezing causes the cells to die and the lesion to fall off or slough off.
Follow-up: The patient is instructed on wound care and given a follow-up appointment to monitor healing and determine if further treatment is necessary.
Cryotherapy is a safe and effective method for removing skin lesions, but it may be associated with some risks and complications, including pain, blistering, scarring, or discoloration. The risks and benefits of cryotherapy are fully discussed in my practice before the procedure.
After cryotherapy, the lesion may form a blister or scab, which will eventually fall off as the skin heals. It is important to protect the area from sun exposure and avoid picking at the scab or blister to prevent infection or further scarring.
Cryotherapy is typically a quick and relatively painless procedure that can be performed in an outpatient setting. It is a good option for removing small, benign skin lesions, but may not be suitable for larger lesions or those suspected to be cancerous or pre-cancerous. The best course of action for skin lesion removal based on the patient’s medical history and the lesion’s characteristics is determined after a full clinical assessment
Laser therapy and electrosurgery
Laser therapy is a method of skin lesion removal that uses a focused beam of light to destroy or remove the lesion. The laser can target the lesion with precision, leaving the surrounding tissue unaffected. Laser therapy is commonly used to remove birthmarks, warts, moles, and other skin lesions.
Topical treatments
Topical treatments are medications that are applied directly to the skin lesion to treat and remove it. Topical treatments are commonly used to remove warts, actinic keratoses, and other benign skin lesions.
Topical treatments for skin lesions can be effective, but they may take several weeks or months to work, depending on the type and size of the lesion. Some topical treatments may cause skin irritation, redness, or discomfort.
Common topical treatments for skin lesions include salicylic acid and 5-fluorouracil (5-FU).
It is important to follow the instructions provided when using topical treatments for skin lesions. The area around the lesion should be kept clean and dry, and the medication should be applied as directed.
Mohs micrographic surgery
Mohs micrographic surgery is a specialized surgical technique used to remove skin cancer and other complex skin lesions. The procedure involves removing the lesion layer by layer, with each layer examined under a microscope until all cancer cells are removed.
Mohs micrographic surgery procedure typically involves the following steps:
Anaesthesia: The patient is given local anaesthesia to numb the area around the lesion.
Removal of the lesion: The surgeon removes the visible portion of the lesion, along with a small margin of surrounding healthy tissue.
Examination of the tissue: The removed tissue is examined under a microscope to determine if all cancer cells have been removed. If cancer cells are still present, another layer of tissue is removed and examined, and the process is repeated until all cancer cells have been removed.
Closure of the wound: Once all cancer cells have been removed, the wound is closed with stitches or other methods.
Follow-up: The patient is given instructions on wound care and given a follow-up appointment to monitor the wound’s healing and determine if further treatment is necessary.
Mohs micrographic surgery is a highly effective method for removing skin cancer and other complex skin lesions, with cure rates exceeding 95%. The procedure allows for the removal of the lesion with minimal damage to surrounding healthy tissue, reducing scarring and other complications.
Mohs micrographic surgery can take several hours or longer, depending on the size and complexity of the lesion.
After Mohs micrographic surgery, the wound may require several weeks to heal. It is important to follow the instructions on wound care, including keeping the wound clean and dry and avoiding strenuous activity until the wound has fully healed.
Risks and Complications
Skin lesion removal is generally a safe and effective procedure, but as with any medical procedure, there are some risks and potential complications. The risks and complications of skin lesion removal depend on the type of procedure used, the patient’s medical history, and the characteristics of the lesion being removed. Some areas of the body, such as the face, as more cosmetically sensitive than others.
Some potential risks and complications of skin lesion removal may include:
Pain or discomfort: Some patients may experience pain or discomfort after the procedure, which can usually be managed with over-the-counter pain relievers.
Bleeding: Bleeding can occur during or after the procedure, especially when the adrenaline wears off. Most bleeding can be controlled with direct pressure and dressing.
Infection: Any procedure that involves breaking the skin can increase the risk of infection. Careful attention to wound care minimises the risk of infection.
Scarring: Skin lesion removal procedures can result in scarring, especially with surgical excision. The risk of adverse scarring can be reduced by the surgical technique, careful tissue handling and by following proper wound care and avoiding sun exposure.
Nerve damage: Skin lesion removal procedures may result in localised numbness or tingling.
Recurrence: In some cases, the lesion may return after it has been removed. Further surgery may be required.
Allergic reaction: Some patients may have an allergic reaction to anesthesia or other medications used during the procedure. This is extremely rare. If you are aware of any allergies, it is important to communicate this to your surgeon.
It is important to discuss the risks and potential complications of skin lesion removal with your surgeon before the procedure. You should also inform your surgeon of any medications, supplements, or medical conditions you have that may increase their risk of complications.
Most risks and complications of skin lesion removal can be managed with proper wound care and follow-up appointments with your surgeon. You should monitor the wound for signs of infection or other complications and seek medical attention if any concerns arise.
Aftercare and Recovery
Wound care
After a skin lesion removal procedure, proper wound care is essential to promote healing and prevent infection. The type of wound care required depends on the type of procedure used and the size and location of the wound. You should follow the wound care instructions provided by your surgeon to reduce the risk of complications and promote optimal healing.
Some general wound care tips after skin lesion removal may include:
Keep the wound clean: You should keep the wound clean and dry to reduce the risk of infection.
Protect the wound: The wound should be covered with a sterile dressing or bandage to protect it from dirt, bacteria, and other contaminants. The dressing should be changed as instructed by your surgeon.
Avoid strenuous activity: You should avoid strenuous activity or exercise that may put strain on the wound, as this can delay healing and increase the risk of complications, including a stretched scar or wound breakdown.
Avoid sun exposure: You should avoid exposing the wound to direct sunlight, as this can increase the risk of redness and discoloration.
Follow medication instructions: If antibiotics or other medications are prescribed, you should follow the instructions provided.
Monitor for signs of infection: You should monitor the wound for signs of infection, such as redness, swelling, warmth, discharge or malodour. If any signs of infection are present, you should contact clinic for review.
Attend follow-up appointments: You should attend all follow-up appointments to monitor the wound’s healing and ensure proper care.
Proper wound care is essential for optimal healing after a skin lesion removal procedure. You should follow the wound care instructions provided and contact your surgeon with any concerns or questions about the wound’s healing process.
Pain management
Pain is a common concern after a skin lesion removal procedure, and you may experience discomfort or soreness for several days after the procedure. Proper pain management can help reduce discomfort and promote a more comfortable healing process.
Some pain management techniques that may be recommended after skin lesion removal may include:
Over-the-counter pain relievers: Over-the-counter pain relievers, such as paracetamol or ibuprofen, can help relieve mild to moderate pain.
Prescription pain medication: If the pain is more severe, prescription pain medication may be indicated.
Ice packs: Applying an ice pack or cold compress to the affected area for 15-20 minutes at a time can help reduce pain and swelling.
Elevation: Elevating the affected area can also help reduce swelling and promote healing.
Relaxation techniques: Relaxation techniques, such as deep breathing or meditation, can help reduce pain and promote relaxation.
Distraction: Engaging in activities or hobbies that are enjoyable can help distract from discomfort and promote a positive outlook.
If the pain is severe or does not improve with pain management techniques, you should contact your surgeon. Pain may be a sign of infection or other complications that require medical attention.
Scar optimisation
Scarring is a common concern after a skin lesion removal procedure, and you may be interested in ways to reduce scarring. Proper wound care and follow-up appointments with your surgeon can help reduce the risk of scarring and promote optimal healing. At the time of surgery, gentle tissue handling, careful technique and choice of sutures minimises scarring.
Some scar prevention and treatment techniques that may be recommended after skin lesion removal include:
Keep the wound clean: Proper wound care can help reduce the risk of infection and promote optimal healing, which can help reduce the risk of scarring.
Avoid sun exposure: Exposing the wound to direct sunlight can increase the risk of scarring and discoloration. Patients should avoid sun exposure or use a sunscreen with at least SPF 30 to protect the wound when it has healed.
Use silicone sheets or gels: Silicone sheets or gels can be applied to scars that become red and raised.
Massage the scar: Massaging the scar gently with a moisturizing lotion can help improve circulation and promote healing, which can help improve the appearance of the scar. This should only be done once the wound has fully healed.
Steroid injections: Steroid injections can be used to improve the appearance of certain scars.
Surgical revision: Surgical revision may be recommended in some cases to improve the appearance of some scars.
It is important to discuss scar treatment options with your surgeon, as the best course of action depends on the size, location, and type of scar.